Cartilage Regeneration: Stanford Study Raises Hope for Natural Knee Repair
A Stanford Medicine-led study has reported a promising advance in cartilage regeneration by blocking a protein linked to aging called 15-PGDH. The study found that an injection inhibiting this protein reversed naturally occurring cartilage loss in the knee joints of old mice and helped prevent arthritis after knee injuries similar to ACL tears. Human cartilage tissue samples from knee replacement surgeries also responded by making new functional cartilage in laboratory conditions.
Why Cartilage Damage Is Hard to Treat
Articular cartilage is the smooth, protective tissue that helps joints move without friction. Once damaged by aging, obesity, injury, or osteoarthritis, it rarely regenerates naturally. Current treatments mainly focus on pain management, physiotherapy, injections, and in severe cases, joint replacement. Stanford Medicine noted that no drug currently slows down or reverses osteoarthritis, making this research highly significant.
The Role of 15-PGDH
The protein 15-PGDH has been described by researchers as a “gerozyme,” a regulator linked to aging and tissue decline. It breaks down prostaglandin E2, a molecule involved in tissue repair. By inhibiting 15-PGDH, researchers increased regenerative signals and helped older joint cartilage behave more like younger cartilage.
Also Read: Dementia Risk Reduction: Regular Physical Activity Linked to 25% Lower Dementia Risk
What the Mouse Study Found
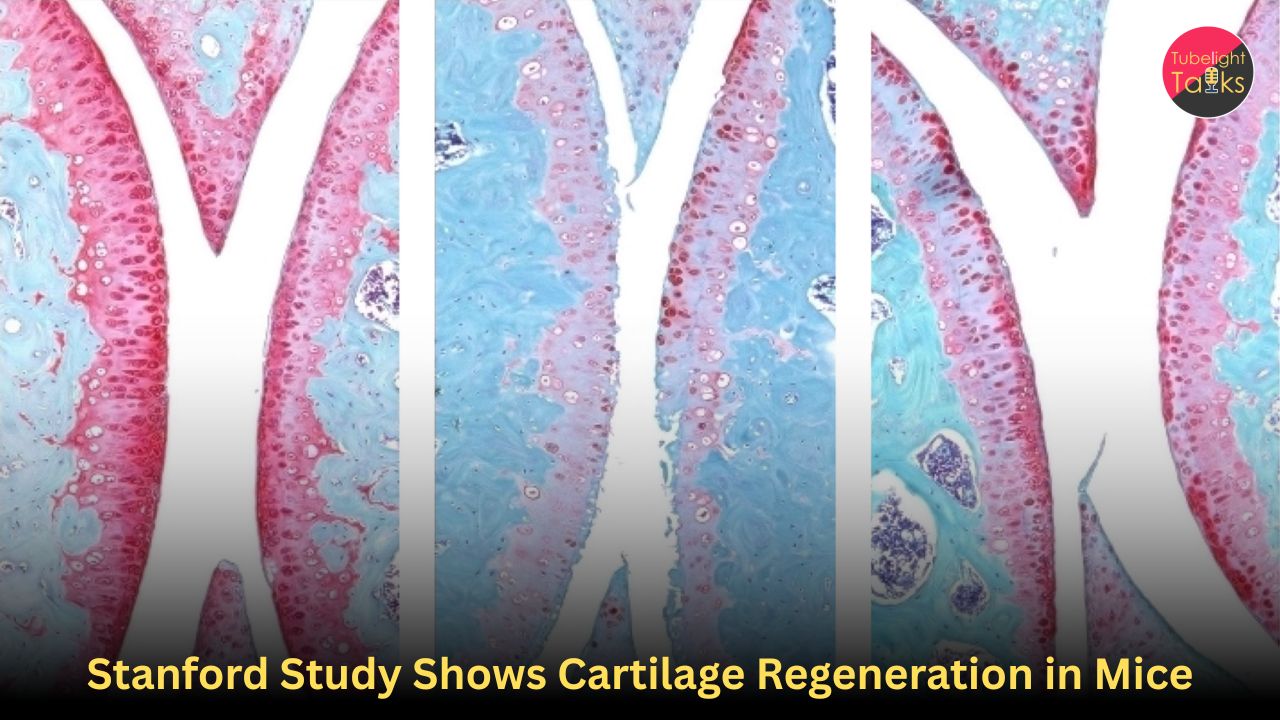
Researchers injected old mice with a small molecule drug that blocks 15-PGDH, both systemically and directly into the joint. In both cases, knee cartilage thickened across the joint surface. Further experiments showed that the new cartilage was hyaline or articular cartilage, the type needed for healthy joint function.
Hope for Injury-Related Arthritis
The research also examined knee injuries similar to ACL tears. Stanford reported that mice receiving injections twice a week for four weeks after injury had a dramatically reduced chance of developing osteoarthritis compared with controls. Treated animals also moved more normally and put more weight on the affected leg.
Human Tissue Response
Human cartilage tissue taken from knee replacement surgeries was treated with the 15-PGDH inhibitor for one week. The tissue showed lower cartilage degradation markers and began regenerating articular cartilage. This is encouraging, but it does not yet mean the treatment is proven in living human patients.
Important Caution
This is a major research milestone, not an approved knee cartilage cure. The strongest results are from mice and laboratory-treated human tissue samples. Human clinical trials specifically for cartilage regeneration will be required to test safety, dosage, effectiveness, and long-term outcomes.
Healing Requires the Right Path
Cartilage regeneration research shows that when the correct cause of damage is identified, healing becomes possible. Sant Rampal Ji Maharaj’s teachings similarly explain that human suffering continues when people follow wrong spiritual practices without scriptural proof. True knowledge identifies the root cause of suffering and guides the soul toward liberation through correct worship. His official teachings emphasize taking refuge in a Tatvadarshi Saint and following scripture-based devotion for complete salvation.
Call to Action
Support Responsible Medical Research
Cartilage regeneration could transform arthritis care, but it must be tested carefully.
Avoid False Cure Claims
Patients with knee pain should consult qualified doctors and follow verified medical guidance instead of relying on unapproved treatments.
FAQs: Stanford Study Shows Cartilage Regeneration in Mice
1. What did Stanford researchers discover?
They found that blocking 15-PGDH regenerated knee cartilage in old mice and human tissue samples.
2. Is this treatment available for humans?
No. It is not yet an approved treatment for human cartilage regeneration.
3. What is 15-PGDH?
It is an aging-linked protein that degrades prostaglandin E2, a molecule involved in tissue repair.
4. Did the study involve human tissue?
Yes. Human cartilage samples from knee replacement surgeries showed regenerative response in lab conditions.
5. Could this reduce knee replacements someday?
Possibly, but only if future human trials confirm safety and effectiveness.









Discussion (0)