Alzheimer’s Treatment Hope: Scientists Find a Way to Help the Brain Clear Harmful Plaques
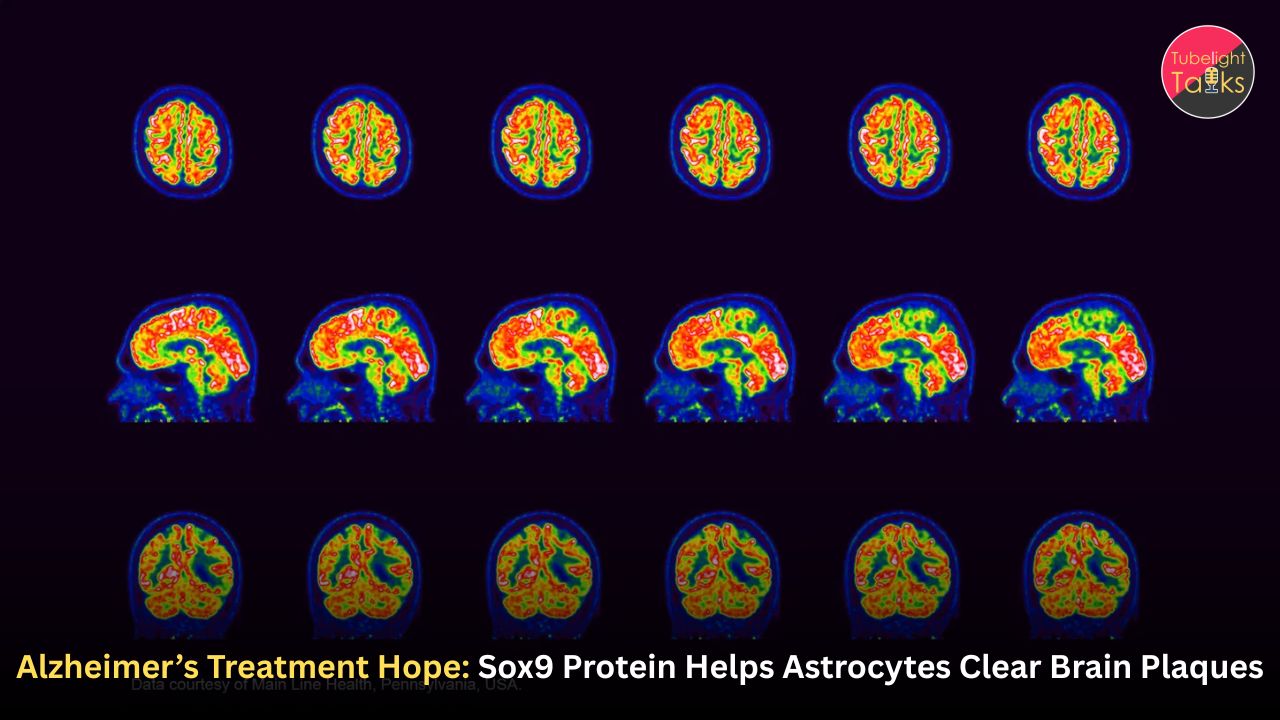
A new Alzheimer’s treatment hope is drawing attention after researchers found that boosting a protein called Sox9 can help the brain’s own support cells clear harmful amyloid beta plaques in laboratory models. The study, led by Baylor College of Medicine researchers and published in Nature Neuroscience, focuses on astrocytes, star-shaped cells that support brain function but are also deeply involved in neurodegenerative disease.
By increasing Sox9 in astrocytes, scientists observed enhanced plaque removal and preservation of cognitive function in Alzheimer’s disease mouse models. The finding does not represent a cure yet, but it opens a promising new direction for Alzheimer’s research.
Alzheimer’s Treatment Hope: Why This Discovery Matters
A Fresh Direction in Alzheimer’s Research
Alzheimer’s disease is one of the most difficult medical challenges of our time because it gradually damages memory, thinking, behavior, and independence. The National Institute on Aging explains that Alzheimer’s-related brain changes involve a complex interplay of abnormal tau, beta-amyloid, inflammation, vascular changes, and other cellular processes, which means the disease cannot be understood through one single pathway alone.
This is why the new Sox9 protein study is important. Most public discussion around Alzheimer’s treatment has focused on amyloid plaques, tau tangles, neurons, and antibody drugs. The latest research adds another possibility: activating astrocytes, the brain’s own support cells, so they can help remove harmful amyloid beta plaques more effectively. Baylor College of Medicine reported that increasing Sox9 expression triggered astrocytes to ingest more amyloid plaques, with senior author Dr. Benjamin Deneen comparing the effect to clearing plaques “like a vacuum cleaner.”
Not a Cure, But a Promising Pathway
This discovery should be understood carefully. The study was conducted in Alzheimer’s disease mouse models and laboratory settings, not as an approved human treatment. Researchers showed that Sox9 overexpression in astrocytes helped clear existing amyloid beta plaques and preserve cognitive function in models of Alzheimer’s disease, but future work is needed before any therapy based on this mechanism can reach patients.
Still, this Alzheimer’s treatment hope matters because it shifts attention from only attacking plaques directly to improving how the brain’s own cells manage plaque buildup. If future research confirms safety and effectiveness in humans, Sox9 protein regulation, astrocyte activation, and the MEGF10 receptor pathway could become part of a new generation of Alzheimer’s therapy strategies.
What Are Astrocytes and Why Are They Important?
The Brain’s Star-Shaped Support Cells
Astrocytes are star-shaped glial cells that perform essential support functions in the brain. They help regulate the environment around neurons, contribute to brain homeostasis, and participate in responses to injury and disease. The Baylor report described them as “brain stars,” highlighting their star-like appearance and central role in supporting cognitive function.
For many years, Alzheimer’s disease research focused heavily on neurons because memory loss and cognitive decline are closely linked with neuronal damage. But astrocytes are not passive background cells. In neurodegenerative disease, astrocytes can become reactive, change their behavior, interact with plaques, influence inflammation, and affect how the brain responds to damage.
Astrocytes as Natural Cleanup Workers
One of the most important findings in the Sox9 study is that astrocytes can phagocytose amyloid plaques. Phagocytosis means a cell engulfs and breaks down unwanted material. In this case, researchers found that enhancing Sox9 helped astrocytes clear amyloid beta plaques through the regulation of MEGF10, a phagocytic receptor involved in the cleanup process.
This matters because Alzheimer’s disease is associated with the accumulation of amyloid beta plaques in the brain. The National Institute on Aging explains that too much beta-amyloid protein leads to plaque buildup, and Alzheimer’s.gov notes that beta-amyloid forms sticky plaques on the brain that can harm brain cells.
The Role of Sox9 Protein in the New Discovery
What Is Sox9?
Sox9 is a transcription factor, meaning it helps regulate the activity of genes. In the new Alzheimer’s research, scientists focused on Sox9 because it is involved in astrocyte function and appears to play a context-specific role in maintaining astrocyte activity in the aging hippocampus and Alzheimer’s disease models. The hippocampus is especially important because it is deeply connected with memory and learning.
Researchers found that increasing Sox9 expression in astrocytes promoted amyloid beta plaque clearance. The study also showed that this mechanism preserved cognitive function in Alzheimer’s disease mouse models, giving the discovery major significance for future Alzheimer’s treatment research.
Sox9, MEGF10, and Plaque Phagocytosis
The mechanism depends strongly on MEGF10, a receptor that helps astrocytes engulf amyloid plaques. The Nature Neuroscience abstract states that Sox9 promotes the phagocytosis of amyloid beta plaques by astrocytes through regulation of the phagocytic receptor MEGF10. In simple terms, Sox9 appears to turn up a cleanup pathway, and MEGF10 helps astrocytes act on that signal.
This gives scientists a more specific therapeutic direction. Instead of broadly stimulating the brain’s immune or support cells, future research may investigate whether the Sox9-MEGF10 pathway can be safely targeted. A treatment that precisely enhances astrocytes’ natural ability to clear plaques could become an important complement to existing amyloid-targeting therapies, although this possibility still requires extensive testing.
How the Study Was Conducted
Alzheimer’s Disease Mouse Models
The research used Alzheimer’s disease mouse models that already showed amyloid plaque buildup and cognitive problems. Baylor College of Medicine reported that the team manipulated Sox9 expression in these models and found that increasing Sox9 helped astrocytes ingest more amyloid plaques.
The published study states that astrocytic Sox9 overexpression cleared existing amyloid beta plaques and preserved cognitive function in Alzheimer’s disease models. This is important because the work did not only examine early prevention; it looked at models where disease-related pathology was already present.
Cognitive Function Preservation
The most hopeful part of the study is not only plaque clearance but also preservation of cognitive function. In Alzheimer’s disease, reducing plaques is valuable only if it helps protect memory and brain performance. The Nature Neuroscience study specifically reported that Sox9 overexpression in astrocytes preserved cognitive function in Alzheimer’s disease mouse models.
This point matters because the Alzheimer’s field has faced a long-standing challenge: amyloid plaque reduction does not always translate perfectly into meaningful cognitive benefit. A pathway that links plaque clearance with better cognitive outcomes is therefore scientifically valuable, even though animal-model results cannot be assumed to work the same way in humans.
How This Discovery Compares With Current Alzheimer’s Treatments
Current Approved Treatments Target Amyloid
In recent years, Alzheimer’s treatment has seen progress through amyloid beta-directed antibody drugs. The U.S. Food and Drug Administration converted Leqembi, also known as lecanemab, to traditional approval in 2023 after determining that a confirmatory trial verified clinical benefit. The FDA described Leqembi as the first amyloid beta-directed antibody converted from accelerated approval to traditional approval for Alzheimer’s disease.
The FDA also approved Kisunla, or donanemab, in 2024 for adults with Alzheimer’s disease. FDA information states that treatment with Kisunla should be initiated in patients with mild cognitive impairment or mild dementia stage disease, which was the population studied in clinical trials.
The Sox9 Approach Is Different
The Sox9 protein discovery differs from these therapies because it does not simply introduce an external antibody to remove amyloid. Instead, it explores whether astrocytes can be activated to perform more effective cleanup inside the brain’s own cellular environment. Baylor College of Medicine noted that most current treatments focus on neurons or on preventing amyloid plaque formation, while this study suggests that enhancing astrocytes’ natural cleanup ability could also be important.
This does not mean Sox9 research replaces antibody drugs. A future Alzheimer’s therapy landscape may include multiple strategies: amyloid-targeting antibodies, tau-targeting treatments, anti-inflammatory approaches, vascular support, metabolic interventions, earlier diagnosis, and cell-specific pathways such as Sox9-MEGF10 astrocyte activation. The NIA’s description of Alzheimer’s as a complex disease supports the idea that multiple biological processes may need to be addressed.
Why Alzheimer’s Is So Difficult to Treat
A Disease That Begins Before Symptoms
Alzheimer’s disease usually begins in the brain years before obvious symptoms appear. By the time memory problems become visible, many biological changes may already be underway. The National Institute on Aging explains that Alzheimer’s-related changes include beta-amyloid plaques, tau tangles, inflammation, and loss of neuronal connections, all of which contribute to progressive brain damage.
This makes treatment difficult because late intervention may not fully reverse damage. Researchers therefore need therapies that can work at different stages: early detection tools, preventive strategies for high-risk groups, treatments that reduce existing pathology, and methods that preserve cognition after symptoms begin.
Plaques Are Important, But Not the Whole Story
Amyloid beta plaques are a key feature of Alzheimer’s disease, but they are not the entire disease. NIA emphasizes that Alzheimer’s involves a complex interplay among abnormal tau and beta-amyloid proteins, inflammation, vascular factors, and other brain changes.
That complexity is exactly why astrocyte-focused research is attracting attention. If astrocytes influence plaque clearance, inflammation, neuronal support, and brain environment, then they may offer a way to address more than one part of the disease process. However, because astrocytes can have both protective and harmful roles depending on context, future therapy must be precise and carefully tested.
Also Read: Brain Mapping Breakthrough: RNA Barcode Technique Reveals the Brain’s Hidden Wiring
What This Means for Patients and Families
Hope With Scientific Caution
For families affected by Alzheimer’s disease, every promising discovery brings hope. But this Sox9 protein study is still at the laboratory stage. It should not be understood as an available treatment, supplement recommendation, or clinical cure. Patients should not attempt any unverified intervention based on this research. Any medical decision should be taken only with qualified healthcare professionals.
The real value of this discovery is that it opens a new therapeutic target. It tells scientists that astrocytes may be more than bystanders in Alzheimer’s disease. They may be active partners in clearing plaques and protecting cognition when the right molecular pathway is strengthened.
Why Early Diagnosis Still Matters
Current FDA-approved amyloid-targeting therapies are intended for early Alzheimer’s disease populations studied in clinical trials, such as mild cognitive impairment or mild dementia stages. This shows why early diagnosis and proper medical evaluation remain essential for patients and caregivers.
If future Sox9-based or astrocyte-based therapies are developed, early diagnosis may again be important because brain cells and circuits may be easier to protect before severe damage occurs. For now, families should focus on medical consultation, evidence-based care, safety planning, caregiver support, and staying informed through authentic health sources.
Future Research: What Needs to Happen Next?
From Mouse Models to Human Relevance
The next major question is whether the Sox9-MEGF10 pathway can be safely and effectively influenced in humans. Mouse models are essential for studying disease mechanisms, but they do not fully capture the complexity of human Alzheimer’s disease. The study included important disease-model findings, but a therapy would require additional preclinical work, safety studies, delivery strategies, dosing research, and eventually human clinical trials.
Researchers must also understand whether increasing Sox9 too much, for too long, or in the wrong cells could create unintended effects. Because transcription factors influence gene networks, therapeutic design must be highly controlled.
Drug Delivery Challenge
Even if the pathway is validated, delivering a treatment to astrocytes inside the brain is a major challenge. The brain is protected by the blood-brain barrier, and many drugs do not easily enter brain tissue. A future therapy might involve gene therapy, small molecules, biologics, RNA-based approaches, or other advanced delivery systems, but each option would need careful testing for safety and effectiveness.
This is why the discovery is a beginning, not an endpoint. The key achievement is that researchers have identified a pathway that may be worth pursuing. Turning that pathway into a patient-ready treatment will take time, evidence, and rigorous clinical research.
Alzheimer’s Research Is Entering a Multi-Target Era
Beyond One-Target Thinking
For decades, Alzheimer’s research has searched for decisive targets that could slow, stop, or reverse the disease. Amyloid remains important, tau remains important, and inflammation remains important. But the field is increasingly recognizing that Alzheimer’s disease likely requires a multi-target strategy. NIA’s overview of the disease supports this view by describing the disorder as involving several interconnected brain changes rather than one isolated defect.
The Sox9 protein discovery fits this new direction. It does not deny the role of amyloid beta plaques. Instead, it asks whether the brain’s own support cells can be guided to manage those plaques better. That is a practical and scientifically grounded question.
Also Read: Hantavirus Outbreak on Cruise Ship: 3 Dead, WHO Probes Cases Near Cape Verde
A New Role for Brain Support Cells
The phrase “brain support cells” can make astrocytes sound secondary, but modern neuroscience is changing that view. Astrocytes help shape the environment in which neurons survive and communicate. In Alzheimer’s disease, their response may influence whether the brain manages damage well or worsens inflammation and degeneration.
By showing that astrocytic Sox9 overexpression can clear existing amyloid beta plaques and preserve cognitive function in disease models, the study gives astrocytes a more central place in Alzheimer’s treatment hope.
Inner Clarity and Care in the Journey of Healing
Medical science searches for ways to reduce suffering in the body and brain, while true spiritual knowledge reminds human beings that inner stability, righteous conduct, and devotion are also essential in difficult times. The teachings of Sant Rampal Ji Maharaj and Sat Gyaan emphasize true worship according to holy scriptures, good karmas, humility, and freedom from harmful practices such as intoxication, dishonesty, violence, and corruption.
In a disease like Alzheimer’s, families often face emotional pain, uncertainty, and long-term caregiving responsibilities. This is where spiritual discipline can give patience, compassion, and moral strength. Just as researchers are discovering that the brain has its own cleanup mechanisms, Sat Gyaan teaches that the soul also needs purification through true worship and correct spiritual guidance. Scientific treatment may support the body and brain, but true devotion gives direction, courage, and the hope of permanent liberation from suffering.
Call to Action: Support Research, Caregivers, and True Knowledge
The Sox9 protein discovery is an important Alzheimer’s treatment hope, but it is not yet an available cure. Patients and families should rely on qualified doctors, authentic medical sources, early evaluation, and evidence-based care. Caregivers should also receive emotional and practical support because Alzheimer’s affects the entire family.
At the same time, everyone should listen to the spiritual discourses of Sant Rampal Ji Maharaj, understand Sat Gyaan, and adopt a life based on truth, discipline, compassion, and true worship. The article structure follows the uploaded Team 5 content style reference.
FAQs on Alzheimers Treatment Hope and Sox9 Protein
1. What is the new Alzheimer’s treatment hope involving Sox9?
Researchers found that increasing Sox9 protein in astrocytes helped these brain support cells clear amyloid beta plaques and preserve cognitive function in Alzheimer’s disease mouse models.
2. Are astrocytes neurons?
No. Astrocytes are glial cells, often described as star-shaped support cells in the brain. They help maintain the brain environment and respond to injury and disease.
3. What are amyloid beta plaques?
Amyloid beta plaques are sticky protein buildups associated with Alzheimer’s disease. NIA explains that too much beta-amyloid can lead to plaque buildup in the brain.
4. What is MEGF10?
MEGF10 is a phagocytic receptor involved in astrocyte plaque clearance. The study found that Sox9 promotes astrocyte phagocytosis of amyloid beta plaques through regulation of MEGF10.
5. Is this Sox9 discovery an approved Alzheimer’s treatment?
No. This is a laboratory and mouse-model discovery, not an approved human treatment. More preclinical and clinical research is needed before any Sox9-based therapy could be used in patients.
6. How is this different from existing Alzheimer’s drugs?
Approved amyloid-targeting drugs such as Leqembi and Kisunla directly target amyloid-related disease processes in early Alzheimer’s populations studied in trials. The Sox9 approach explores whether the brain’s own astrocytes can be activated to clear plaques more effectively.









Discussion (0)